Advanced Spine Surgery gets Coloradans Back on Path | by

Catherine Vrba had been an athletic person all her life, especially devoted to long distance running. But after two car accidents, she started to experience back pain that increased in frequency and severity over several years. Everyday activities such as looking after the house, driving her children where they needed to go and walking the family’s two dogs became almost unbearable.
“Every year, the pain would get worse,” Vrba recalls. “I’d think, ‘Well, I’ll see my chiropractor again or go for more massage,’ but the pain went to my leg and became excruciating. I couldn’t stand up straight and was using a walker on rollers. Even lying down became painful.”
“This is cutting edge, and we’re very fortunate to have one in Colorado. I think it’s a real game changer.”
Limited mobility, let alone constantly managing acute pain with medication, was no longer an option for Vrba, 40, who has three children. She had to rely on others for help with driving and household activities. Sometimes, even though her job in a church was sedentary, she’d have to leave work early. “My husband did all the housework,” she says. Vrba also had to drop out of a course she was taking toward a master’s degree.
Last April, Vrba’s primary care physician referred her to Dr. Zak Ibrahim, a surgeon at South Denver Spine. Ibrahim, a spine surgeon for 16 years, nonetheless didn’t immediately recommend surgery. “I’m conservative,” he says. “We try everything before surgery—physical therapy, injections and chiropractic treatment, among other modalities.”
The important thing for people to understand, Ibrahim says, is that most back pain isn’t dangerous, and surgery is always a last option. “But it’s also important for people to understand that surgery can be a very good option and they shouldn’t be afraid of it.”
Vrba wasn’t afraid. “We tried the injections and several MRIs, and Dr. Ibrahim told me he would be as conservative or as aggressive as I wanted him to be.” In her case, structural damage to the vertebra, combined with debilitating pain that impeded everyday activities, qualified surgery as the right option. Knowing her life had to change, Vrba underwent surgery in September 2013.
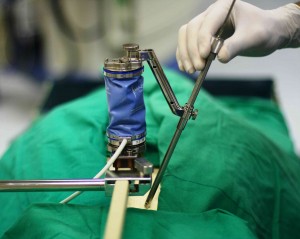
Ibrahim used a form of robotic guidance called Mazor Renaissance™ to repair the structural damage to Vrba’s spine, which included a stenosis, or narrowed, lumbar vertebra. The way Ibrahim explained it, the technology didn’t faze Vrba. “It was interesting,” she says. “Knowing how precise things could be, I was comfortable. It was advancement.”
“The primary application for the Mazor technology — which I consider wonderful technology — is for minimally invasive surgeries and patients with severe deformities such as scoliosis, kyphosis, or structural injuries,” Ibrahim says.
To repair Vrba’s injury, Ibrahim had to remove what was left of the vertebra, implant screws and plates to stabilize her spine, and then use synthetic bone to fill the gap. Of course, any reconstructive spine surgery will require planning and precision, and there are other robotics systems out there. But the Mazor Renaissance computerized guidance level of precision is “uncanny,” Ibrahim says. There are about 25 Mazor systems being used in the US. “This is cutting edge, and we’re very fortunate to have one in Colorado. I think it’s a real game changer.”
Here’s how it works: Using the system’s virtual 3-D environment, the surgeon creates a blueprint, or template, to plan where the instrumentation, or surgical tools, will go.
Next, the surgeon mounts a guide to the patient’s spine, which ensures accurate placement of the implants (such as screws or plates).
Once the mount is complete, the surgeon next uses fluoroscopy, or moving X-ray images, of the patient’s spine, to synchronize to the preoperative blueprint. That’s where the “uncanny” precision comes in.
When the blueprint and CT scan are synchronized, the tools and implants are guided according to the plan.
What this means for the patient is less time in surgery: What would have taken about four hours for a procedure like Vrba’s took about one and a half hours. And because the surgeon uses a 3-D blueprint, the patient’s exposure to radiation is significantly reduced. Trauma to surrounding soft tissue around the spine also is minimized, so recovery is faster, and the patient can get up and get moving more quickly, Ibrahim says.
Catherine Vrba returned to work part time just two weeks after surgery. By October she was back to work full time. She and her husband take their dogs, an Australian Shepherd and a Rottweiler/Shepherd mix, for a mile walk after work, and Catherine is working with a physical therapist to get back up to running speed. Ibrahim is confident that in time she’ll resume long-distance running.
“I don’t think I’ll be running a marathon anytime soon,” Vrba says, “but a half-marathon might be doable.”
Visit: www.southdenverspine.com for more information.
Tags: spine surgery
Leave a Comment
Please be respectful while leaving comments. All comments are subject to removal by the moderator.